If you’re caring for someone with limited mobility, learning how to use air mattress for bedsores could prevent painful pressure ulcers before they develop. Medical air mattresses work by continuously redistributing body pressure, preventing the sustained compression that restricts blood flow and causes tissue damage. For family caregivers and healthcare professionals alike, understanding the proper setup, adjustment, and monitoring of these specialized surfaces makes the difference between healthy skin and serious wounds requiring extensive treatment. This practical guide delivers the specific techniques you need to maximize protection against bedsores using air mattress therapy.
Clinical evidence confirms that appropriate air mattress use significantly reduces pressure ulcer incidence among vulnerable populations. According to National Institute for Health and Care Excellence (NICE) guidelines, pressure redistribution devices are essential for high-risk patients. Whether you’re managing care at home or in a healthcare facility, mastering these evidence-based techniques ensures you’re providing optimal protection while reducing your overall caregiving burden. This guide covers the exact steps you need to implement air mattress therapy correctly for bedsore prevention.
How Air Mattress Pressure Redistribution Prevents Bedsores
Medical air mattresses combat bedsores through alternating pressure technology that automatically shifts weight distribution across the body. When pressure remains constant on bony areas like hips, heels, or tailbone, blood vessels compress, restricting oxygen delivery to tissues. Without adequate circulation, skin and tissue begin dying within hours, leading to painful pressure ulcers. The alternating inflation and deflation cycles in therapeutic air mattresses solve this problem by ensuring no body area remains under constant pressure.
Key physiological benefits you’ll achieve:
– Continuous blood flow restoration to previously compressed tissues
– Reduced tissue oxygen deprivation that causes cell death
– Prevention of the sustained pressure that initiates ulcer formation
– Enhanced healing capacity for existing minor skin damage
The alternating pressure cycle typically operates on 5-10 minute intervals, mimicking the natural repositioning movements mobile people make unconsciously. As air cells inflate and deflate in coordinated patterns, pressure redistributes across the body surface, allowing blood flow to temporarily restore to compressed areas. This continuous cycle provides therapeutic pressure relief without requiring constant manual intervention, making it especially valuable during overnight care when repositioning frequency would otherwise decrease.
Why Standard Mattresses Fail for Bedsore Prevention
Conventional foam or spring mattresses create dangerous pressure points that concentrate force on bony prominences. When you lie still, these pressure points restrict blood flow to vulnerable areas while surrounding tissues receive adequate circulation. This uneven distribution creates the perfect conditions for bedsores to develop within hours. Medical air mattresses eliminate this problem through dynamic pressure redistribution that maintains more even support across the entire body surface.
Selecting Your Ideal Air Mattress: Alternating Pressure vs. Low Air Loss

Choosing the right air mattress type directly impacts your bedsore prevention success. Understanding the differences between alternating pressure and low air loss systems ensures you select equipment matching your specific care needs and patient risk factors.
Alternating Pressure Mattresses for General Prevention
For most bedsore prevention scenarios, alternating pressure mattresses provide the optimal balance of effectiveness and accessibility. These systems feature individual air cells that inflate and deflate in coordinated patterns, typically changing pressure distribution every 5-10 minutes throughout day and night. The alternating action ensures no single body area remains under constant pressure, providing therapeutic relief without requiring manual intervention.
Look for these essential features:
– Adjustable pressure settings based on patient weight
– Cycle timing controls (5-15 minute intervals)
– Dual-mode operation (alternating pressure and static inflation)
– Automatic pressure compensation for position changes
These mattresses work best for patients with moderate risk factors who need continuous pressure redistribution but don’t have significant moisture management challenges. They’re generally more affordable than low air loss systems while providing excellent preventive benefits.
Low Air Loss Mattresses for High-Risk Patients
If your patient experiences incontinence, excessive sweating, or lives in warm environments, low air loss mattresses provide critical additional protection. These specialized systems incorporate microclimate control through continuous airflow that carries away perspiration while maintaining optimal skin temperature. The dry, cool environment significantly reduces the secondary risk factor of moisture that weakens skin integrity.
When to choose low air loss systems:
– Patients with incontinence issues
– Individuals who sweat heavily during sleep
– Care in warm or humid environments
– Existing stage 1-2 pressure ulcers requiring aggressive prevention
The constant air circulation through the mattress surface prevents moisture accumulation that would otherwise soften skin and accelerate pressure damage. While typically more expensive, this moisture management capability makes low air loss systems essential for high-risk patients where standard alternating pressure mattresses might fall short.
Step-by-Step Air Mattress Installation for Maximum Protection
Proper installation determines whether your air mattress delivers therapeutic benefits or creates hazardous conditions. Follow these specific steps to ensure safe, effective setup that maximizes bedsore prevention.
Pre-Installation Bed Frame Preparation
Before placing your air mattress, thoroughly prepare the bed frame to prevent damage and ensure even support. Remove all bedding and inspect the frame surface for sharp edges, protruding hardware, or accumulated debris that could puncture the mattress. Measure carefully to confirm mattress dimensions match or slightly exceed the bed frame to prevent dangerous gaps where body parts could contact hard surfaces.
Critical installation checks:
– Confirm bed frame stability (no wobbling or shifting)
– Remove all sharp objects from the sleeping surface
– Verify frame dimensions against mattress specifications
– Ensure adequate space for pump placement and tubing access
An improperly prepared surface undermines the therapeutic benefits of even the most advanced air mattress system. Taking 5-10 minutes for proper preparation prevents equipment damage and ensures consistent pressure redistribution.
Correct Pressure Settings for Your Patient’s Weight
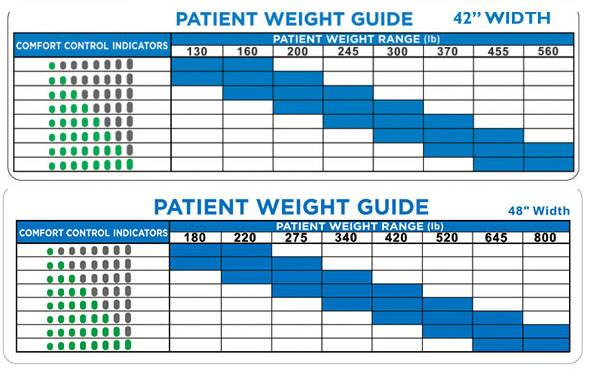
Setting appropriate air pressure based on patient weight is the most overlooked yet critical factor in bedsore prevention. Lighter patients (under 150 lbs) typically require lower pressure settings to achieve adequate immersion without creating new pressure points, while heavier patients need higher pressures to prevent excessive sinking.
Follow this pressure adjustment protocol:
1. Inflate mattress to manufacturer’s recommended starting pressure
2. Have patient lie in normal sleeping position for 15 minutes
3. Slide hand under patient’s lower back – should fit with slight resistance
4. If hand slides in easily, increase pressure incrementally
5. If hand cannot slide in, decrease pressure slightly
6. Recheck after 1 hour of use and adjust as needed
Incorrect pressure settings render even the best air mattress ineffective for bedsore prevention. Too little pressure allows body parts to sink deeply, concentrating force on bony areas, while excessive pressure reduces the effectiveness of alternating cycles. Document your final pressure settings for future reference and adjustment.
Daily Monitoring and Maintenance Protocols
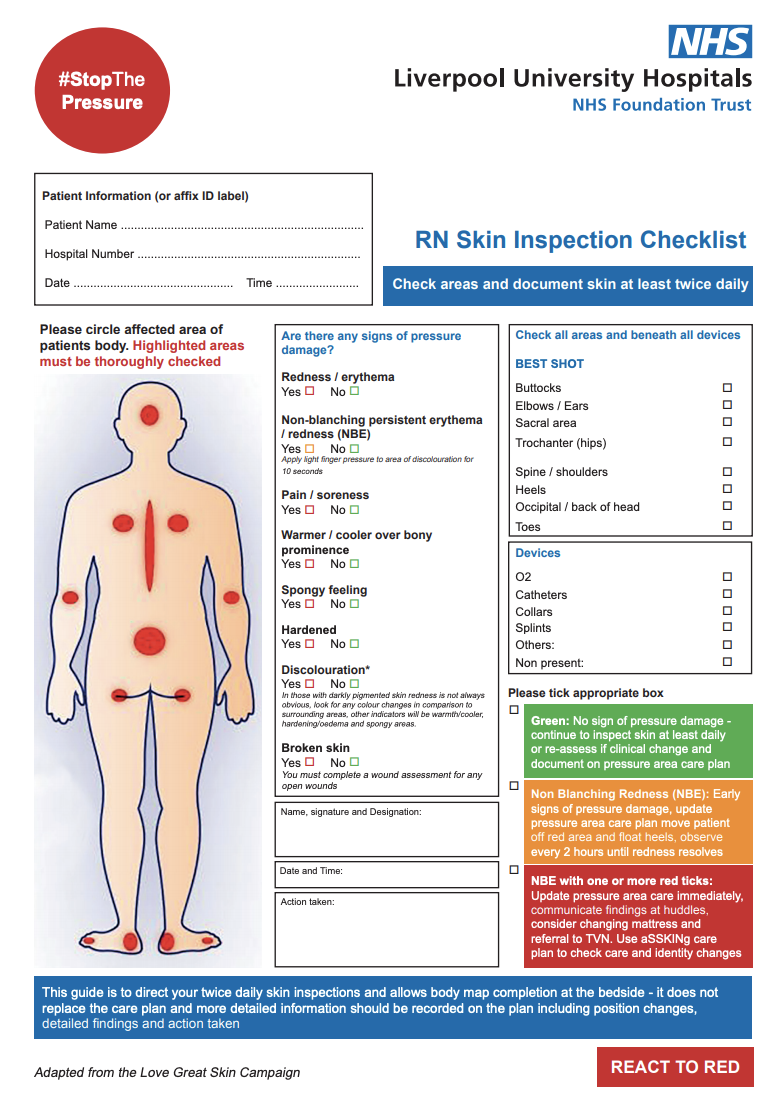
Proper air mattress use requires consistent monitoring and maintenance to ensure continuous therapeutic effectiveness. These daily practices protect vulnerable skin while extending equipment lifespan.
Essential Skin Inspection Routine
Conduct systematic skin inspections at least twice daily, focusing on high-risk areas where bedsores most commonly develop. The hips, tailbone, heels, elbows, and back of the head require particular attention as these bony prominences experience the highest pressure concentration.
What to look for during skin checks:
– Areas of persistent redness that don’t fade within 20 minutes of pressure relief
– Skin that feels warmer or cooler than surrounding areas
– Swelling or changes in skin texture
– Blisters, breaks in skin integrity, or unusual discoloration
Early detection of stage 1 pressure damage (non-blanchable redness) allows immediate intervention before progression to more serious wounds. Document findings with precise location descriptions to track changes over time and identify patterns requiring equipment adjustment.
Troubleshooting Common Air Mattress Problems
Air leaks represent the most frequent equipment problem that compromises bedsore prevention. Locate leaks by applying soapy water to suspected areas – bubbling indicates the leak source. Small punctures can often be repaired with manufacturer-provided patch kits, while larger damage may require professional repair.
Immediate action steps for common issues:
– Air leaks: Isolate leak source, apply temporary patch, schedule permanent repair
– Incorrect pressure: Recheck weight-based settings, make incremental adjustments
– Pump malfunctions: Consult error code guide, reset if appropriate, contact support
– Moisture accumulation: Verify low air loss function, increase room ventilation
Maintain a backup manual air pump for emergencies to ensure continuous pressure redistribution if primary equipment fails. Never leave high-risk patients without appropriate pressure-relieving support for extended periods.
Maximizing Protection with NHS-Recommended Practices
Following NICE guidelines ensures your air mattress use aligns with evidence-based best practices for bedsore prevention. Quality Statement 8 specifically recommends pressure redistribution devices for high-risk individuals, establishing medical air mattresses as standard care.
Combining Air Mattress Therapy with Repositioning
Even with effective pressure redistribution, incorporate regular repositioning into your care routine. NICE guidelines recommend position changes every 4 hours for patients using alternating pressure mattresses, compared to every 2 hours without. This reduced frequency still provides additional pressure relief while enabling thorough skin inspection.
Optimal repositioning schedule:
– Morning: Full skin inspection and position change
– Midday: Quick skin check at 90-degree turn
– Evening: Full skin inspection and position change
– Night: Minimal disturbance while verifying pressure redistribution
This combined approach provides superior protection compared to either intervention alone, addressing multiple pathways to tissue damage while supporting comprehensive skin health.
Maintenance Schedule for Long-Term Effectiveness
Establish a consistent maintenance routine to ensure your air mattress continues delivering therapeutic benefits throughout its service life. Daily visual inspections, weekly deep cleaning, and monthly functional testing prevent problems before they compromise patient care.
Preventive maintenance checklist:
– Daily: Check for visible damage, verify proper inflation, inspect skin condition
– Weekly: Clean surface with approved disinfectants, check tubing connections
– Monthly: Test alternating pressure cycles, verify pressure settings accuracy
– Quarterly: Professional equipment assessment and calibration
Proper maintenance extends equipment lifespan while ensuring consistent therapeutic effectiveness. Document all maintenance activities to track patterns and identify emerging issues before they affect patient care.
Maintaining appropriate pressure settings, conducting regular skin inspections, and addressing equipment problems promptly protects at-risk individuals from painful pressure damage while reducing caregiving burden. When used correctly as part of a comprehensive prevention strategy that includes proper nutrition, moisture management, and regular repositioning, medical airflow mattresses provide effective protection that allows patients to rest comfortably while their skin remains healthy and intact. By following these evidence-based techniques aligned with NHS guidelines, you’ll maximize the therapeutic benefits of air mattress therapy for bedsore prevention in your care environment.